Lyme disease is an infectious disease transmitted by the bite of an infected western blacklegged tick. It is caused by a spirochete (Borrelia burgdorferi) that may persist in the human body for several years if not treated with antibiotics. The natural history of this disease is not completely understood and the illness it produces takes many forms. Because of varied symptoms, diagnosis can be difficult. This newly recognized disease was first noted in 1975 at Old Lyme, Connecticut, and was first seen in California in 1978.
Lyme disease is now recognized as an important tick-borne disease throughout the northeastern USA from Massachusetts to Delaware; in the Midwest in Minnesota and Wisconsin; in some southeastern states; and in the west in California, Oregon, and Nevada, as well as in many European countries.
The Vector of Lyme Disease in California
The western blacklegged tick, which is known to transmit Lyme disease, has been found in many areas of Ventura County. Heaviest concentrations of ticks have been in the humid coastal areas and along horse and hiking trails.
The western blacklegged tick (Ixodes pacificus) is the only tick of the 49 species occurring in California that is known to transmit Lyme disease. The spirochete causing Lyme Disease was first isolated from this tick in 1984.
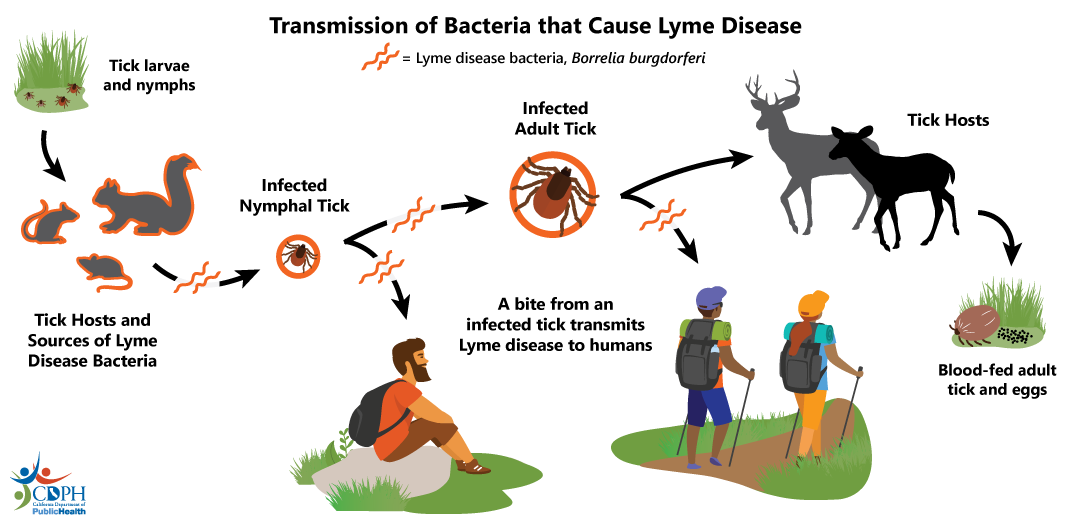
The western blacklegged tick has three active life stages: Larva, nymph, and adult.
-
Larval and nymphal western blacklegged ticks acquire spirochetes from the blood of infected mammals as they feed. Immature stages (larvae and nymphs) feed on small rodents, rabbits, lizards, birds, and occasionally large mammals. Once infected, nymphs and adults can transmit the spirochetes to other mammals (including humans). In California, a low percentage of the ticks tested are infected with the Lyme disease spirochete.
-
Adult western blacklegged ticks are most commonly found from December through June, during the period of the year when humidity is usually high. The adult female is red-brown with black legs, about 1/8 of an inch long; males are smaller and entirely brownish black. Both are teardrop shaped. Adults feed on large mammals, including deer, dogs, and humans.
-
All stages feed by embedding their mouth-parts into the skin of a host and taking a blood meal.
-
An infected western blacklegged tick must be attached to a person and feed for at least 24 hours before it can transmit the bacteria that cause Lyme disease.
The western blacklegged tick can typically be found on grasses and brush in both urban and rural settings. Ticks do not fly, jump, or drop from the trees. Instead they climb to the tips of vegetation, typically along animal trails or paths, and wait for a host to brush against them. This behavioral method of finding a host is called questing.
Symptoms
Lyme Disease commonly has these three stages:
- Stage 1
The first recognizable symptom usually is a characteristic rash, erythema chronicum migrans (ECM), that occurs 3 to 30 days after the bite of an infected tick. ECM is a red, blotchy, circular, expanding rash that may grow to several inches in diameter and clears centrally, producing a ring-like appearance. One or more ECM lesions may occur, not necessarily at the tick bite site. ECM may be preceded or accompanied by flu-like symptoms. These symptoms may persist, change, disappear and reappear intermittently for several weeks. - Stage 2
Some infected persons may develop long-term complications weeks to months after the initial symptoms. These complications may include disorders of the heart or nervous system. Abnormalities of the heart include varying degrees of blockage of the heart muscle. Nervous system abnormalities include meningitis, encephalitis, facial paralysis (Bell's palsy) and other conditions involving peripheral nerves. During this stage, patients may experience migratory pain in joints, tendons, muscles, and bones, often without joint swelling or redness. - Stage 3
Months to years after disease onset, patients may develop arthritis that appears and disappears intermittently for several years. Arthritis is the most common long-term symptom of Lyme disease. Large joints, especially the knees, are the most often affected. Lyme arthritis may become chronic, with erosion of cartilage and bone.
What to do if you think you have Lyme Disease
Early recognition of Lyme disease is important. If you have found a tick attached to your skin or if you have been in an area where ticks are known to occur and if you have any of the symptoms listed above, tell your physician immediately. This information, together with a blood test, will help your physician make a diagnosis.
Treatment with antibiotics during the early stages can cure the infection and prevent the complications associated with stages 2 and 3. Antibiotic treatment of the later stages of Lyme disease is often, but not always, successful.
For additional information on Lyme disease contact the Ventura County Environmental Health Division at 805/654-2816.
Tick Avoidance
Personal
- Tuck pants into boots or socks, and shirt into pants.
- Wear light-colored clothing so ticks can easily be seen.
- Apply insect repellent on pants, socks, and shoes. Use a repellent registered for use against ticks.
- Avoid trail margins, brush, and grassy areas when in tick country.
- Check yourself and your children frequently.
Environmental
- Mow grass along buildings and footpaths.
- Remove brush in areas of high human activity.
- Area application of insecticides is not effective for tick control.
Removal of Attached Ticks
- Prompt removal of ticks may prevent disease transmission
- If possible, have someone else remove the tick from you.
- Use tweezers or forceps rather than your fingers.
- If you must touch the tick, use a tissue to protect your hand.
- Exposure to the body fluids of the crushed or squeezed tick may lead to transmission of Lyme or other disease agents.
- Grasp the tick's mouth-parts as close to the skin as possible.
- Gently pull the tick straight out, steadily and firmly. Do not twist or jerk the tick.
- Tick mouth-parts have harpoon-like barbs; they do not screw into the skin.
- If mouth-parts of the tick break off and remain in your skin, consult your physician.
- Dispose of tick in alcohol or by flushing it down the toilet.
- Wash hands and bite site with soap and water. Apply antiseptic to bite site.
